Patient FAQs
General
What is the purpose of blood-thinners in heart disease?
- Blood thinners prevent the development of a thrombus (blood clot) within the body
- Once a thrombus forms, it can block various chambers or blood vessels and/or break off, becoming an embolism, where it can then travel through the blood stream and lodge in an artery elsewhere within the body (thrombo-embolism)
- Specific types of blood thinners are indicated for specific reasons
- Hence one or more categories of blood thinners may be required in certain situations
- The benefit of using blood thinners (reducing clotting) must always be balanced with risks (bleeding).
Why do I need to take blood thinners after my procedure?
- There are two types of blood thinners: antiplatelets and anticoagulants.
- Depending on your individual factors and the procedure you had, you may have to take a combination of these medications.
- These medications help to make your blood less sticky, preventing it from forming clots.
- Blood clots can be dangerous, as they can stop the blood from flowing, potentially leading to a heart attack or stroke.
What are the different types of blood thinners used in heart disease?
- Oral Anti-Coagulants (OAC) – pills taken by mouth to reduce formation of fibrin (mesh) within the blood
- Warfarin (Coumadin) – requires regular blood tests, which measure how long it takes your blood to clot (INR) . Dose varies according to INR value.
- NOAC (or DOAC) means novel or direct oral anticoagulant– consists of once or twice daily pills that do not require frequent monitoring e.g. apixaban, edoxaban, rivaroxaban and dabigatran
- Injectable/Intravenous Blood-Thinners
- used in hospital in emergency situations
- occasionally injectable agents used out-of-hospital (low molecular weight heparin – e.g.. Dalteparin, Enoxaparin)
- Anti-Platelet Therapy (APT) – prevent “sticky platelets” from forming clot
- Aspirin (ASA)
- P2Y12 Blockers (Clopidogrel, Ticagrelor, Prasugrel)
- Dipyridamole (persantine)
- Combination Therapy
- Blood thinners are very specific; certain blood thinners protect against clotting in specific circumstances and in certain situations combination therapy is necessary
- ASA may be combined with a P2Y12 Blocker
- ASA and/or a P2Y12 blocker may be combined with an OAC
- If atrial fibrillation is present and a stent has been inserted into a coronary artery, then a combination of anti-platelet medication (P2Y12 Inhibitor +/- Aspirin) will be needed for stent protection, and a Novel Oral Anti-Coagulant (eg. NOAC) may be necessary for the Atrial Fibrillation
- Duration of the anti-platelet medication will vary based on individual factors
What are the signs and symptoms of stroke?
- Call 911 immediately if you experience any of these signs/symptoms
- REMEMBER FAST
- Face: is it drooping?
- Arms: can you raise both?
- Speech: is it slurred or jumbled?
- Time: to call 911 right away
- Act fast because the quicker you act, the more of the person you save.
What are the signs and symptoms of a heart attack?
- Call 911 immediately if you experience any of these signs/symptoms
- Chest Discomfort (pressure, squeezing, fullness or pain, burning or heaviness)
- Upper Body Discomfort (neck, jaw, shoulder, arms back)
- Sweating
- Shortness of Breath
- Feeling lightheaded
- The most common sign is chest pain or discomfort in men and women
- Women can experience a heart attack without chest pressure
- Women may experience:
- Pressure/ pain in lower chest or upper abdomen
- Dizziness/ Light-Headedness/ Fainting
- Upper Back Pressure
- Extreme Fatigue
What are the signs and symptoms of bleeding?
- If you experience any of these signs, see prompt medical attention or call 911
- Symptoms of stroke
- Sudden severe headache and/or neck stiffness
- Confusion
- Dizzy, vertigo (spinning sensation)
- Faint or lightheaded
- Confusion
- Loss or blurry vision
- Short of breath
- Low blood pressure and/or fast heart rate
- Bloody or black (tarry) stools
- Vomiting blood or coffee-like material
- Coughing up blood
- Blood in urine
- Pain, swelling, reduced motion in a major joint
- Swelling and major bruising such as thigh, arm or abdominal wall
- Sudden pain in the chest, abdomen, flank or back
- Bleeding that doesn’t stop with compression such as a nosebleed
What can I do to reduce the risk of bleeding?
- Take medications as prescribed
- Maintain regular medical follow-up (in the case of warfarin, your doctor will arrange for regular blood tests to monitor INR)
- Ensure blood pressure is well-controlled
- Avoid anti-inflammatory medication (unless prescribed by a doctor)
- Any new medication should be confirmed with your doctor and pharmacist to ensure no adverse interaction with blood thinners
- Caution about over-the-counter medicines or herbal supplements that have effect on blood thinning (e.g. tumeric, garlic, ginkgo biloba). Check with a pharmacist to be certain
- Limit or avoid alcohol (or at least excessive or binge drinking). Maximum 1 oz spirits, 12 oz. beer or 1 glass wine per day if you do drink.
- Notify doctor if any dental or medical or surgical procedures are scheduled
- Caution or avoidance of activities at high risk of falling or trauma
- Recognize the signs/ symptoms of bleeding
- See special precautions for those taking warfarin
What do I do if I am scheduled for a procedure or operation after discharge?
- Ensure your cardiac specialist, doctor or dentist doing the procedure is aware of your heart condition and medications – especially blood thinners
- In some cases of minor procedures the blood thinners can be continued, but in more invasive surgery they may need to be stopped (the specialist and cardiologist should be informed and provide guidance on any alteration of dosing, when to stop and resume after the procedure)
- Occasionally an injectable anticoagulants may be used for a few days when warfarin is temporarily discontinued to reduce the risk of clotting under the guidance of your physician
- Certain dental and medical procedures and surgery may require a dose of antibiotic (usually pills) to be taken before the operation to protect against infection (especially those with artificial heart valves, certain congenital heart defects, transplanted hearts and other heart devices). Coronary stents, in most cases, alone do not require such antibiotic coverage.
Atrial Fibrillation
What is Atrial Fibrillation ?
- The heart creates its own electrical impulse called sinus rhythm which is a regular rhythm usually at a rate between 50-70 beats per minute at rest, increasing to higher rates depending on exercise or activity, anxiety, etc.
- Atrial Fibrillation is a common heart rhythm disorder, whereby the upper chamber of the heart (atrium) causes the heart to beat in an irregular rhythm beat-to-beat and it is often at a faster rate unless medication is utilized.
How does Atrial Fibrillation lead to blood clots and stroke ?
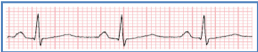
Normal Sinus Rhythm:
- Blood flowing (red circles) into the left atrium from the lungs is pumped into the left left ventricle (LV) when the heart is beating in regular (sinus) rhythm (Fig. 1).

Fig.1
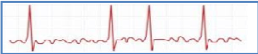
Atrial Fibrillation:
- When the heart rhythm becomes irregular (in atrial fibrillation or flutter), the left atrium ceases to empty properly and blood can stagnate in the atrial pouch (or appendage ), potentially leading to clot formation (Fig. 2).

Fig. 2
- The clot that forms in the left atrium can potentially dislodge and travel in the blood stream, eventually lodging in an artery elsewhere. If it travels to the brain it can cause a stroke (Fig. 3).

Fig. 3
- The clot that forms in the left atrium can potentially dislodge and travel in the blood stream, eventually lodging in an artery elsewhere. If it travels to the brain it can cause a stroke (Fig. 3).
Do all patients with atrial fibrillation have a risk of stroke?
- The risk of stroke in patients with atrial fibrillation or flutter depends various factors
- Age (65 or above), diabetes, high blood pressure, heart failure, previous stroke or transient ischemic attack(TIA), are all factors which determine stroke risk referred to as “CHADS” risk factors.
- The more factors present, the greater the stroke risk
What medications are required to reduce the risk of stroke in atrial fibrillation ?
- If age is less than 65 years and there are no CHADS risk factors, then the risk of stroke is low. Aspirin may be all that is required.
- If age is over 65 years and/or there is one or more CHADS risk factor, then the risk of stroke is increased, and generally an oral anticoagulant is required
- If at any age, the atrial fibrillation is associated with a valve damaged by rheumatic fever, Warfarin is required.
Blood Thinners & Bypass Surgery
What blood thinners are needed following coronary bypass surgery?
Following Coronary Artery Bypass Graft (CABG) you will require blood thinners.
This may be as simple as aspirin, or Aspirin + a P2Y12 agent
Aspirin may be combined with an oral anti-coagulant (OAC) if Atrial Fibrillation is present.
Blood Thinners & Heart Valves
What blood thinners are required for mechanical heart valves?
Mechanical heart valves require protection against clot formation. If the valve is a mechanical (metal) valve then Warfarin (and usually aspirin) are necessary (Fig. 1).

Fig. 1
What blood thinners are required for cow/pig (tissue) or TAVI heart valves?
For a surgically implanted cow or pig valve, Warfarin may be used for 3 months (healing period), then aspirin alone.
TAVI valves require anti-platelet agents (aspirin and clopidogrel) for 3 months, then a single agent alone (Fig. 2).
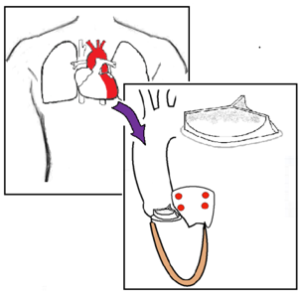
Fig. 2
If there is a reason for anti-coagulant therapy, such as atrial fibrillation, then an OAC (NOAC or Warfarin) may be combined with the anti-platelet therapy necessary for the valve itself (Fig. 3).
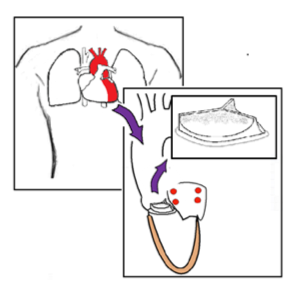
Fig. 3
LV Thrombus
Can a blood clot form within the heart itself?
Clots can form in the left ventricle (LV) chamber of a weakened heart or following a large heart attack (myocardial infarction).
Warfarin is the preferred medication for variable period of time.

Blood Thinners & Other Procedures
What blood thinners are needed following other devices in the heart (LVAD, occluding devices, mitra-clip)?
Other heart devices including valve clips, occluding devices and heart pump assist devices (Left Ventricular Assist Devices – LVADs) require blood thinners that will be specified by the cardiologist and heart surgeons.

Blood Thinners & Coronary Artery Stents
What blood thinners are needed for a coronary artery stent?
Stents are implanted in the arteries of the heart to reduce chest pain (angina), or during the course of a heart attack to improve blood flow.
They require anti-platelet therapy (Aspirin + P2Y12 agent) for a specified period of time to prevent blood clots within the stent (which can cause a heart attack).
If there is a reason for anti-coagulant therapy, such as atrial fibrillation, then an OAC (NOAC or Warfarin) will be combined with the anti-platelet therapy (necessary to prevent clotting due to the stent).

Blood Thinners & Pulmonary Embolisms
What blood thinners are needed for a blood clot in the lung (pulmonary embolism)?
Clots in the Leg (DVT or Deep Venous Thrombosis) can break off and lodge in the Lung (Pulmonary Embolism, or “PE”).
Oral anticoagulants (OAC) or occasionally injectable anticoagulants are needed.

Warfarin
What is INR?
- International Normalized Ratio (INR) is a measure of the time it takes blood to clot (a higher INR means the blood takes longer to clot).
- Normal INR is 1 (0.9-1.1)
- Warfarin increases the INR and the usual range for treatment is between 2-3 (occasionally up to 3.5) depending on the condition treated
- When warfarin is initiated, it may take several days to reach the target range of INR
Vitamin K and green leafy vegetables can lower the INR and make blood more prone to clot - Other medications (especially antibiotics) can alter the INR either up or down) depending on the agent
- INR can also be elevated in certain conditions such as liver disease
What do I need to know about Warfarin ?
- Warfarin (or Coumadin) is an oral blood thinner that works by blocking formation of blood clotting molecules produced by your liver
- These molecules (called clotting factors) are regulated by vitamin K; hence, taking vitamin K (or excessive green leafy vegetables, a natural source of vitamin K) will interfere with Warfarin’s effect, making your blood more likely to clot
- Take Warfarin exactly as prescribed, and take it at the same time every day with or without food
- Maintain regular INR blood tests as ordered and become familiar with the level. Adjustments in dose will be made if necessary from your doctor or other designated medical personnel
- If you forget the dose, take it later the same day. If you forget to take that day altogether, resume the usual dose the next day. Missing 2 days in a row should prompt a check of INR
- Any new medications, over-the-counter products or herbal/dietary supplements, should be discussed with your doctor, nurse practitioner and/or pharmacist to determine the potential effect on INR (see Reducing Risks of Bleeding)
- Avoid or at least minimize alcohol intake (maximum 2 per day) and avoid binges
- Avoid anti-inflammatory agents (such as ibuprofen, naproxen) as they increase the risk of bleeding
- Other blood thinners such as Aspirin, clopidogrel, ticagrelor, prasugrel, dipyridamole (persantine), increase the risk of bleeding and are utilized only under the direction of a physician
- Occasionally an injectable anticoagulants may be used for a few days when Warfarin is temporarily discontinued, to reduce the risk of clotting under the guidance of your physician
- Warfarin is never used along with a NOAC (DOAC)
- If you have signs of bleeding or another illness seek medical attention
- Notify doctor if any dental or medical or surgical procedures are scheduled
- If you become pregnant, notify your physician
- Caution or avoidance of activities at high risk of falling or trauma
- A medical alert bracelet is recommended